For many, jails are the only place to access mental health care, but once inside, the conditions of prison life may exacerbate mental illness and reduce the likelihood of rehabilitation. Mentally ill people should have access to care in prison, and advocacy for mental health care should extend beyond the concerns of prison conditions.
For many, jails are the only place to access mental health care, but once inside, the conditions of prison life may exacerbate mental illness and reduce the likelihood of rehabilitation. Mentally ill people should have access to care in prison, and advocacy for mental health care should extend beyond the concerns of prison conditions.
The Imparity of Mental Health Care in Prison
- Category: Uncategorized
- Tags: capacity | criminal-responsibility | mental health | prison | PTSD | violence
- Date: March 25, 2014
- Author: admin2
Justices Hear Florida Case on Measuring Inmates’ Mental Disabilities
 WASHINGTON — A majority of the Supreme Court seemed skeptical on Monday of how Florida decides who is eligible to be spared the death penalty on account of intellectual disabilities. The state uses an I.Q. of 70 as a rigid cutoff, and several justices suggested that it should take account of a standard margin of error or consider additional factors.
WASHINGTON — A majority of the Supreme Court seemed skeptical on Monday of how Florida decides who is eligible to be spared the death penalty on account of intellectual disabilities. The state uses an I.Q. of 70 as a rigid cutoff, and several justices suggested that it should take account of a standard margin of error or consider additional factors.
Other justices seemed inclined to allow Florida and other states to decide for themselves how to determine who is “mentally retarded” and so ineligible for execution under the court’s 2002 decision in Atkins v. Virginia.
The Atkins decision gave states substantial discretion and only general guidance. It said a finding of intellectual disability requires proof of three things: “subaverage intellectual functioning,” meaning low I.Q. scores; a lack of fundamental social and practical skills; and the presence of both conditions before age 18. The court said I.Q. scores under “approximately 70” typically indicate intellectual disability.
As Monday’s argument progressed, it became clear that what divided the two groups of justices was more than the particular case. Their disagreement was a larger one about the role of scholarly and professional expertise in the resolution of legal disputes.
Read the full article, Justices Hear Florida Case on Measuring Inmates’ Mental Disabilities, in New York Times. By Adam Liptak, March 3, 2014. See more coverage of this issue in the article, With Death Penalty, How Should States Define Mental Disability?, on NPR. By Nina Totenburg, March 3, 2014.
- Category: News
- Tags: capacity | Competency | criminal-responsibility | death penalty | expert witness | law | violence
- Date: March 4, 2014
- Author: admin2
Scammers take aim at aging population
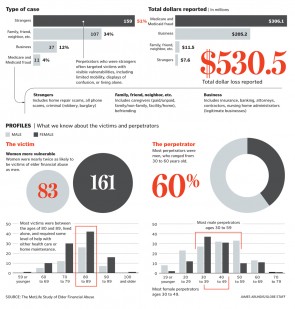
Elder financial abuse
Researchers analyzed media reports from April through June 2010, and pinpointed 314 unduplicated reports of elder financial abuse that included detailed information. Source Metlife Study on Elder Financial Abuse. Credit: James Abundis, Boston Globe.
By Kay Lazar | The Boston Globe | January 6, 2014
Roughly 21,000 times last year, physicians, social workers, family members, and other concerned residents contacted Massachusetts Protective Services authorities to report suspicions that an elderly person was being abused.
In about one third of those cases, the concern involved financial exploitation, according to state officials, a problem that is expected to grow significantly as the population ages and the number of older adults left vulnerable by Alzheimer’s disease nationwide is projected to double, and perhaps triple, by 2050.
With a potential tsunami of elder financial abuse on the horizon, researchers, health care leaders, lawyers, and lawmakers have launched a number of initiatives to better understand the size and scope of the issue and craft strategies to minimize harm. Continue reading »
- Category: Press
- Tags: Boston Globe | capacity | decision-making | elders | Rebecca Brendel
- Date: January 7, 2014
- Author: The Boston Globe and admin2
Watch: Capacity, Finances, and the Elderly: Brain Science Meets the Law
On December 12th, 2013, at Brigham and Women’s Hospital’s Bornstein Amphitheater, CLBB joined forces with the Boston Society of Neurology and Psychiatry to host a conversation among experts in neurology, psychiatry, and the law about how the science of aging could impact how we protect older adults from victimization and undue influence. Where do we draw the line between protection and paternalism? What constitutes a bad financial decision? Who needs additional protections?
Panelists included Bruce H. Price, MD, Chief of Neurology at McLean Hospital and Co-Director of CLBB; Rebecca W. Brendel, MD, JD, Consultant to the Law & Psychiatry Service at MGH, Clinical Director of the Home Base Program, Assistant Professor of Psychiatry, Harvard Medical School; Susan Stenger, Attorney with decades of experience handling probate litigation, including undue influence and lack of capacity cases; and Judge Susan Ricci, Associate Justice of the Massachusetts Probate and Family Court in Worcester.
Kay Lazar, Health Reporter at the Boston Globe with a focus on Aging, Sports Medicine and Public Health, moderated a panel discussion and Audience Q&A following the speaker remarks.
To watch video from this event, visit our Vimeo channel on Capacity, or watch individual segments below.
Also, read Kay Lazar’s story about this topic and CLBB’s role in the Boston Globe.
- Category: Events
- Tags: capacity | Competency | decision-making | elders | finances | undue influence
- Date: December 15, 2013
- Author: admin2
Cognitive Impairment and Decision Making in the Elderly at AAPL 2013
As the incidence of cognitive impairment increases with advancing age, a larger number of our elderly population will suffer some variety of dementing disorder. Causes include Alzheimer’s disease, multi-infarct dementia, and a variety of other disease states. Effects can vary to very subtle to severe. At some point, cognitive impairment may limit an elder adult’s ability to make decisions. These limits may be in specific domains, such as financial or medical.
 Alternatively, cognitive limitations may be more global in nature. Some elder adults had the foresight to record specific beliefs prior to any cognitive disease. Health care proxies, living wills, or financial power of attorney document an individual’s choices at an earlier time point.
Alternatively, cognitive limitations may be more global in nature. Some elder adults had the foresight to record specific beliefs prior to any cognitive disease. Health care proxies, living wills, or financial power of attorney document an individual’s choices at an earlier time point.
But many adults do not put their wishes in writing. Also, adults are free to change their opinion at any point. The question must then be asked: at what point does cognitive impairment limit a person’s capacity to make decisions? There is not one simple answer. The level of scrutiny varies with the task. For example, making changes to a will generally only requires a low level understanding of one’s estate and heirs. Other tasks, such as consenting to a complicated medical treatment, will require far more understanding. Thus, the level of scrutiny is much higher. But where should society draw the line between protection and paternalism?
These and other issues were addressed by a panel at this year’s Annual Meeting of the American Academy of Psychiatry and the Law (AAPL), which took place in San Diego, California on October 24-27, 2013. The panel, entitled “Impaired Medical Decision-Making in Older Patients,” included a lively discussion between Stephen Read, M.D. of the Department of Psychiatry and Biobehavioral Sciences at UCLA; Debra Pinals, M.D., the Assistant Commissioner of Forensic Services for the Massachusetts Department of Mental Health; Phillip Resnick, M.D., the Director of the Forensic Psychiatry Fellowship at Case Western Reserve; Sherif Soloman, M.D., an Assistant Professor of Psychiatry at Case Western Reserve; and Robert Weinstock, M.D., the Director of the UCLA Forensic Psychiatry Fellowship Program.
- Category: Uncategorized
- Tags: AAPL | capacity | Competency | decision-making | elders
- Date: November 9, 2013
- Author: Eric Huttenbach